- Home
- Guidelines
- Innovation
-
Education
- Study Days & Courses
- STAR Simulation App
- Faculty Resources
- Videos >
- Respiratory Videos (High flow, Tracheostomies, Chest drains, and sleep studies)
- Speciality Training Resources
- Paediatric Long Term Ventilation Team
- Life Support Resources
- #PedsCards Against Humanity
- Bronchiolitis Surge Resources
- Other Educational Opportunities
- Research
- Conference
-
Trainees
- Preceptorships
-
Networks
- Wessex Children's and Young Adults' Palliative Care Network
- PREMIER - Paediatric Regional Emergency Medicine Innovation, Education & Research Network
- Wessex Allergy Network
- Wessex Paediatric Endocrine Network
- Wessex Diabetes Network
- Clinical Ethics >
- TV and Wessex Neonatal ODN
- Regional Referrals to Specialist Services >
- Search
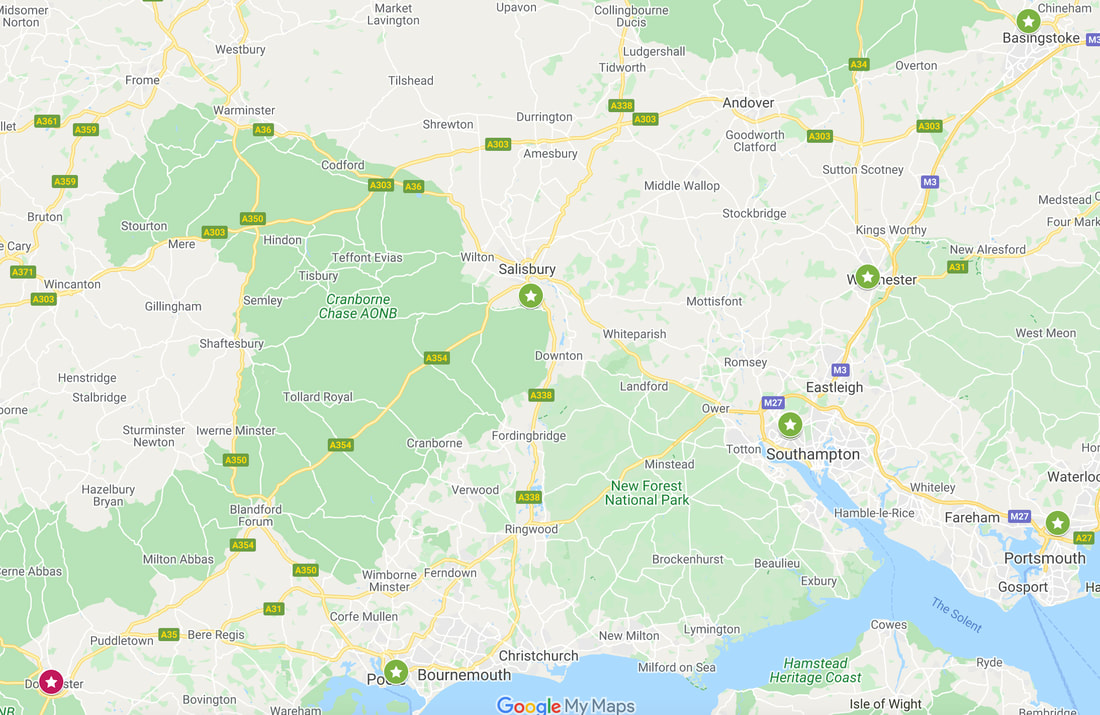
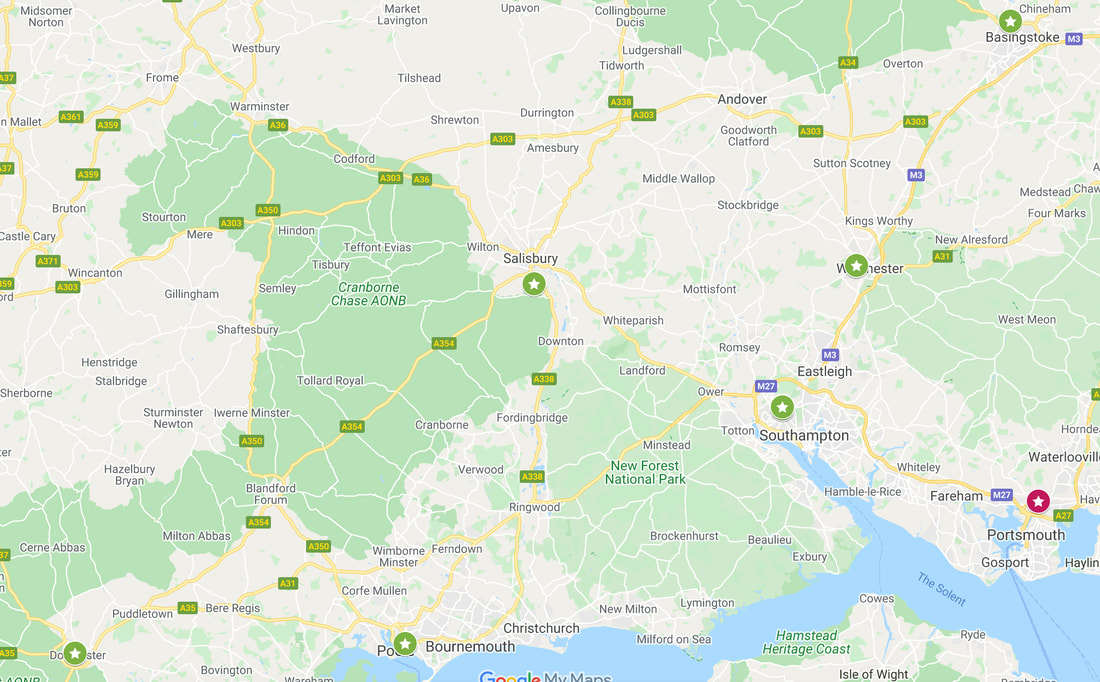
A rough-guide to the different placements in the region, helping you decide how to rank your rotation options
All the information is complete to the best of our (and our helpers) knowledge, we apologise for any errors or omissions. If you have specific questions or want more information then those colleagues currently in each placement will be able to advise further and the trainee reps are also happy to advise or direct you to people who can help.
All the information is complete to the best of our (and our helpers) knowledge, we apologise for any errors or omissions. If you have specific questions or want more information then those colleagues currently in each placement will be able to advise further and the trainee reps are also happy to advise or direct you to people who can help.
- Jemma Shanley, Wessex Trainee Rep RCPCH trainee committee ([email protected])
- Shreya Chugh ST1-3 School Board Rep ([email protected])
- Debora Calderoni ST1-3 School Board Rep ([email protected])
- Basingstoke and North Hampshire HospitalBasic info
- Ward = approx. 20-24 beds (depending on staffing) + HDU (one bed)
- Charlie’s assessment unit = 6 beds, takes referrals from GP & A&E
- Neonatal unit has 6 ITU cots + several SCBU places.
- PAU in the emergency department is staffed periodically with Paediatric consultants.
Features- Busy district general with a large patient load, which provides lots of opportunities and experience
- Systems in place to help manage large work load, for example all the nursing staff on Charlie’s can do bloods, cannulas.
- SHO mix of F2/GPST and ST1 paediatric trainees.
- Limited priority given to clinic experience on the rota.
- Mix of in region trainees, and long standing specialist doctors, ENP and Consultants to share wealth of knowledge but also different ways to manage conditions which may be hard for developing as new registrar.
- All wards, outpatient and offices including community are all on one floor of the hospital so easy access and good collaboration between acute team, consultants, community and therapists.
Community- Vast range of experiences on offer; MASH visits, looked after children clinics, behavioural support, early intervention based in schools, sleep clinic, ophthalmology, adoption panels, sexual abuse service and much more all signposted and eager to welcome you to shadow.
- Trainee lead in allocating times to see new referrals and completing developmental assessments with good senior support for advice.
- Self motivation and good organisation needed to ensure timetable filled.
Rota lead- Tara Brown ([email protected])
- Ward = approx. 20-24 beds (depending on staffing) + HDU (one bed)
- Dorset County HospitalBasic info
- Kingfisher Ward: 14 beds + Paediatric Assessment Unit (6 beds + treatment room). Day surgery patients on adjacent ward.
- Level 1 Neonatal Unit: 5 HDU cots
Features- Clinic experience timetabled into rota (~12 per 6 months); some remote locations (Bridport, Weymouth, Blandford) so car transport key.
- Trauma Unit with helipad - HEMS do bring patients if not stable for bypass to Southampton.
- Supportive consultant body and Anaesthetics department; they are used to managing patients in-house as PICU is further away.
- One Kingfisher ANNP and one SCBU ANNP who mostly work normal working hours - an invaluable support
- SHOs a mix of F1s, F2s, GP trainees and trust doctors
- Less neonatal experience as only those >32 weeks are planned for (can be the occasional unplanned preterm delivery though).
- Quieter unit with the occasional very sick patient - a good ST3 step-up placement as usually there’s time to think and consider decisions and a supportive consultant body.
- There’s opportunity to be involved in lots of clinics and other meetings and non-clinical opportunities.
- Admin time also given for clinics
- Can claim excess mileage and accommodation costs (variable availability of on-site accommodation) via HEE Relocation Policy (Support provided with organising this)
Community- Based on site in the separate outpatient Children’s Centre alongside therapy teams so able to shadow.
- Given regular clinics early on but mainly follow up patients
- Weekly school visit/clinics run across the county; own transport needed.
Rota lead- Emma Garland ([email protected])
- Kingfisher Ward: 14 beds + Paediatric Assessment Unit (6 beds + treatment room). Day surgery patients on adjacent ward.
- Poole NHS Foundation TrustBasic Info
- Wards (Acrewood & Bearwood) = 26 beds (including 4 HDU beds)
- Children’s assessment unit (Elmwood) = 9 beds, takes referrals from GP & ED (also from Bournemouth ED – as no inpatient paediatrics there)
- Day case ward for day case theatre, infusions/injections and PJS - nurse run
- Small paediatric area in Poole ED – run by ED team
- Neonatal unit – run separately from general paeds in St Mary’s
- Maternity Hospital
- Level 2 unit: 4 ITU cots, 6 HDU cots, 10 SCBU cots
- Run by ANNPs & consultants - general paeds registrar provides emergency support out of hours (does mean the occasional jog across the road)
Features- Busy district general with a large patient load, which provides lots of opportunities and experience Systems in place to help manage large work load, for example majority of nursing staff and HCAs can do bloods (and some also do cannulas – particularly on CAU)
- All wards, outpatient and consultant offices are all on one floor of the hospital so easy access and good collaboration between acute team and other consultants
- Well supported by therapy services including physio & dietetics
- SHO mix of F2/GPST and ST1 paediatric trainees
- At least 2 x blocks of clinic weeks per 6 month placement given to SHOs + other opportunities
- Regular rapid access and alongside consultant clinics for registrars (general & sub-speciality)– with specified admin time!
- Well suited for all registrars – particularly senior trainees to expand clinic experience and ‘acting up’
- SPIN opportunities: Cardiology, HDU, community/neurodisability
Community- Based at Children’s Development Centre on site but separate from acute wards
- Also community clinics at Pelham and Moordown
- Run by a mixture of experienced consultants and associate specialists – all very supportive
- Consultants lead on all inpatient & outpatient safeguarding cases and provide on call service 24/7
- Vast range of experiences on offer; MASH visits, looked after children clinics, behavioural support, special school clinics, adoption panels, sexual abuse service and much more all signposted and eager to welcome you to shadow
Rota Lead- Dr Sumit Bokhandi ([email protected]) – usually supported by a registrar
Admin Lead- Wendy Edwards ([email protected]) – facilitates registrar clinic rota
- Queen Alexandra HospitalGeneral Paediatrics
Basic Info- Wards Starfish (medical) =24 beds & Shipwreck (surgical) = 18 beds
- Children’s assessment unit (CAU)= 15 beds, 2 stabilisation rooms, takes referrals from GP, Paeds ED & directly from paramedics (except trauma, surgical issues, mental health issues & patients receiving active CPR)
- Day case work done on CAU on Thursdays/Fridays led by nurses
- Dedicated Paediatric ED – run by Paeds ED consultant/ junior staff separate from general paeds staffing between 8am – 2am
- Neonatal unit – run separately from general paeds
- Level 3 unit: 14 ITU beds, 8 HDU beds, 32 SCBU beds
- Run by neonatal team – Consultants, Paediatric trainees, F2 & ANNPs. Rarely can be called for extra help
Features- Very busy district general with a large patient load, which provides lots of opportunities and experience
- Systems in place to help manage large work load, for example majority of nursing staff are very experienced & can do bloods & cannulas – particularly on CAU. Consultants often stay on till late to manage workload.
- All wards, outpatient and consultant offices are all on A level of the hospital so easy access. 2 x hot week consultants during the week (one for the ward/ one for CAU). Excellent team working amongst the consultants to support busy work load.
- Well supported by allied health professional teams including pharmacists, physios & dieticians
- SHO mix of F2/GPST/ Military GP trainees and ST1 paediatric trainees
- SHOs will have weeks on CAU/ ward/ Paeds ED. Prolonged jaundice clinic run by SHOs twice a week supervised by consultants.
- Registrars are expected to attend consultant clinics in the morning on their LD shifts before their CAU shift.
- Well suited for all registrars – particularly in learning to manage acutely unwell children and busy workload.
- Very supportive and competent local ITU team in managing sick children.
- SPIN opportunities: HDU, Diabetes & Endocrine, Cardiology
Rota Lead- Dr Lou Collins ([email protected]) and Louise Milne ([email protected]) – usually supported by a registrar
Admin Lead- Charlene Murray ([email protected]) - Junior doctor co-ordinator
Community
Basic info- Based at Portsmouth city, Havant & Fareham. One trainee per location but lots of opportunity to work between sites.
- On-call shifts based on CAU, Starfish & Shipwreck
Features- Run by a mixture of experienced consultants and associate specialists – all very supportive
- Safeguarding is covered by Community team between 9am-5pm, out of hours will be referred to general paeds
- Vast range of experiences on offer; Neurodisability clinics, MASH visits, looked after children clinics, behavioural support, special school clinics, adoption panels, sexual abuse service, joint CAHMS clinics and much more all signposted and eager to welcome you to shadow
Community lead- Dr Danielle Rowley ([email protected])
Neonates
Basic info- Tertiary referral Neonatal Unit with approximately 550 admissions a year
- 14 intensive care cots, 8 high dependency cots, 10 special care cots
- Bliss Baby Charter
- Located on Ward B9 on B level
- Labour Ward and Maternity Theatres are located next to the unit, with the Postnatal Ward and Mary Rose Midwifery led unit also on B level and accessible through Labour Ward.
- In addition to the paediatric trainees there are currently 2 ANNPs on the registrar rota and 2 ANNPs and 2 F2s on the SHO rota
Features- Very consultant-led and often consultant-delivered service so a supportive environment for a first neonatal registrar post. They will be there in the middle of the night if needed!
- Your time will be split between the NICU, HDU/SCBU, and PNW
- Excellent opportunities to learn how to manage complex neonatal cases and extreme preterm infants
- Lots of opportunities for procedures (intubation, longlines, umbilical lines, LPs, CrUSS) initially for the registrars, then ST3s and then ST1s
- Excellent teaching programme
- In the unit: weekly trainee-led teaching, consultant-led teaching (including SIM), journal club
- Joint with the General Paediatric Team: weekly Grand Round
- Joint with the Maternity Team: monthly Perinatal M&M
- Opportunity to teach medical students
- Opportunities to get involved with audit, QI and to do GCP so you can get involved with the research projects the unit is recruiting for.
- Charlotte Groves ([email protected])
- Royal Hampshire County HospitalBasic info:
- Ward (Northbrook) - 2 base x6 + 7 cubicles currently (total 19)
- Assessment unit (Sophie's Place) - Approx 13 beds open day time all week (shorter hours at weekends).
- Neonatal Unit (Level 2) - covered by general paeds. 2 ICU cots, 2 HDU cots and 8 SCBU cots.
- Paediatric area of ED - accessible to staff opposite Northbrook ward. 3 bed spaces plus mental health room.
- There is usually an additional consultant as ‘flow’ to help with flow from ED to PAU. This reduces pressure on registrars taking calls from ED as well as doing WR and jobs.
Features:- Generally a popular choice of rotation due to central location in deanery, friendly staff and good training opportunities (PAFTAs training unit of the year 2019)
- SHOs - F2/GPVSTs and some staff grades, ANP + 2 ANNPs. Consultants do resident nights.
- Consultant & secretary offices, as well as registrar office/night break room all near NNU. Of note this is across the car park from the main children’s ward.
- Safeguarding medicals usually seen by general on-call team
- Teaching: 2 formal sessions/week (junior and consultant led) plus X ray meeting and regular neonatal SIM (mainly aimed at SHOs).
- Limited priority given to regular general paediatric clinic experience on rota at present
- Increasing nurses/HCAs training in cannulation & phlebotomy on Ward, Assessment unit and Neonates.
- Recommended step up ST3 job - consultants very used to having new registrars and are approachable, and either live closeby or will stay onsite overnight.
Community:- Opportunities to do neurodevelopmental clinics, observe autism assessments as well as adoption & LAC clinics, school clinics, nursery observations, enuresis clinic, early years social communication group meetings.
- Opportunities to shadow other members of MDT
- Also covers clinics in Andover & Eastleigh
- Opportunities to observe sexual abuse service in Basingstoke
- On general paeds teaching rota
- Good organisational skills key to use time efficiently
- Trust laptop available to join Teams meetings/do admin etc.
Rota lead- Deb Pathak ([email protected])
- Salisbury NHS Foundation TrustBasic Info:
- Initially built by the US army as a WWII rehab hospital so it’s a bit of a maze to get around – use ‘Sarum entrance’ for paeds ward
- Ward (Sarum): 16 beds
- Day Assessment Unit (Woodlands): 5 beds and large waiting/play area. Open daytime hours only.
- Takes referrals from GP & ED, plus daily consultant rapid access reviews Mon-Fri
- Level 2 Neonatal Unit – run by general paediatricians
- 4 ITU/HDU cots, 10 SCBU cots (4 are brilliant kangaroo care rooms)
Features:- District general with a moderate patient load, capturing patients from a large area including 3 counties (Hampshire, Dorset & Wiltshire) – so they can take quite a while to arrive after referral!
- Regional children’s burns and plastics unit (including cleft palate/lip) – excellent opportunities to have experience of, and learn more about these areas
- Ongoing close military ties and serves the children of several military bases/patches
- Lots of consultant-supported clinic experience (~20 per 6 months)
- You will also get the opportunity to run Registrar clinics with 8-10 patients in a session with a mix of new and follow up patients.
- Paediatric wards directly above outpatients & consultant offices so easy access and good collaboration between acute team and other consultants
- More long days, fewer night shifts as consultants cover quite a few night shifts
- SHOs are a mix of F2s, GP trainees and trust doctors
- Opportunities to take part in child protection reviews/medicals, strategy meetings and write reports, all with consultant support
- Particularly well suited for ST3 registrar stepping up in 1st registrar role and senior registrar in preparation for CCT.
Community:- No community placements here as outsourced to VirginCare
- Therapy services also managed by VirginCare but based on site and are very helpful – referral mechanism is slightly different, but you will be guided by the consultants.
Rota Lead- Dr Tracey Farnon ([email protected])
- University Hospital SouthamptonBasic info:
- Major tertiary Children’s hospital, including PICU and Children’s ED.
- Research centre in partnership with University of Southampton.
- Registrar placements in SPIN/GRID specialties.
- Rotation of ST2: 6 months in PICU or Cardiology and 6 months in specialities:
- Respiratory, Nephrology, Gastroenterology, Oncology,
- Neurology, Surgery, Endocrinology.
G- Floor- Regional centre for all specialities; wealth of clinical experience and cases not often seen elsewhere in the region- good for clinical examination preparation!
- Very busy, particularly over winter, with multiple teams and MDTs involved in patients.
- Opportunities to be involved in research and QI projects, peer teaching, and mentoring medical students.
- SHOs will be allocated a specialty as their ‘base’ team, but may occasionally be asked to cross-cover other specialties. The out-of-hours rota covers all specialties. SHOs will have allocated time in the Children’s ED.
Rota leads- James Edelman ([email protected]) and Annie Goss ([email protected])
Paediatric Intensive Care Unit- A leading paediatric intensive care unit providing services across the south of England and Channel Islands and in conjunction with
- Oxford providing retrieval services as far north as Milton Keynes Hospital.
- Centre for cardiac surgery; opportunity to really understand cardiac anatomy and physiology looking after these patients post operatively.
- Intense environment but supportive team, lots of educational opportunities both on the unit and set aside teaching days.
- Working alongside a mixed team of PICU GRID, adult anaesthetic/ITU, paediatric emergency medicine GRID, and fellow paediatric trainees; learning from each other.
- Supported to achieve transport competencies and take part, potentially leading your own paediatric retrievals in registrar placements.
Rota lead- Mel Connett (ANP) ([email protected])
Cardiology- Regional referral centre for all cardiology linked with PICU, NICU across the road and John Radcliff hospital Oxford.
- A chance to see lots of cardiac patients; good for clinical exam practice.
- Registrar rota is very heavy and whilst always reachable, and often taking lots of calls, overnight they may go off-site which can leave the SHO covering the ward alone (with PICU support close at hand).
Rota lead- Najih liagathali ([email protected]) or Norah Yap ([email protected])
Community- Base office is a large shared office with all members of the community team, including admin, therapy services, health visitors etc. Clinics are held across the city in RSH and health centres. Own transport is helpful as you may be in multiple places throughout the day.
- You are given a work laptop and mobile phone to allow working across different sites and from home
- You are on the child protection on-call rota which means seeing a range of different child protection cases but always with another senior doctor (standard practice to have 2 doctors during a medical)
- Most clinic experience is running your own neurodisability clinics with lots of opportunity to attend LAC clinics, special school clinics, general paeds clinics, therapy sessions, adoption panels.
- On calls are in Southampton children’s ED.
Neonates- As one of the largest neonatal units in the country, they treat around 900 babies a year, from across the South and the Channel Islands.
- 23 intensive and high dependency cots and 14 special care cots
- SONeT base for Transport of Neonates across the region.
- Maternity Theatres, Labour ward, Postnatal Ward and Midwife led unit (Broadlands) are located within the Princess Anne within close proximity of the neonatal unit.
- Opportunities to manage Cardiac and Surgical Babies, as Southampton has paediatric surgery and paediatric cardiology & cardiac surgery on site.
- Large MDT including dietician, psychology, pharmacy dedicated to the unit
- Rostered time split between SCBU, NICU, Postnatal ward and clinics (and transport for Registrars)
- Usually a well-staffed rota, 2 Registrars and 2 SHOs on a night shift with a mix of regional trainees, MTI trainees and ANNPs on the Junior doctor rota.
- Princess Anne is across the road from PICU and Radiology so sometimes this requires babies to be transferred via ambulance for surgery or radiology, this can cause delays but there is a system in place to facilitate this.
Rota lead- Sarah Davidson ([email protected])
- Major tertiary Children’s hospital, including PICU and Children’s ED.
PIER Contact |
|
- Home
- Guidelines
- Innovation
-
Education
- Study Days & Courses
- STAR Simulation App
- Faculty Resources
- Videos >
- Respiratory Videos (High flow, Tracheostomies, Chest drains, and sleep studies)
- Speciality Training Resources
- Paediatric Long Term Ventilation Team
- Life Support Resources
- #PedsCards Against Humanity
- Bronchiolitis Surge Resources
- Other Educational Opportunities
- Research
- Conference
-
Trainees
- Preceptorships
-
Networks
- Wessex Children's and Young Adults' Palliative Care Network
- PREMIER - Paediatric Regional Emergency Medicine Innovation, Education & Research Network
- Wessex Allergy Network
- Wessex Paediatric Endocrine Network
- Wessex Diabetes Network
- Clinical Ethics >
- TV and Wessex Neonatal ODN
- Regional Referrals to Specialist Services >
- Search